When conservative treatments no longer relieve shoulder pain or restore movement, shoulder replacement surgery, also known as arthroplasty, may offer a path toward renewed function and comfort. One of the most important considerations is understanding reverse total shoulder vs total shoulder arthroplasty. In this post, we’ll take a look at these two procedures, outlining when each is typically recommended and what patients can generally expect during recovery.
Key Takeaways
- A total shoulder replacement mimics the natural anatomy: a plastic socket replaces the glenoid (shoulder socket), and a metal ball replaces the humeral head (arm bone).
- The “reverse” name in reverse shoulder replacement comes from the altered anatomy: the metal ball is fixed to the shoulder socket, and the plastic socket is placed on the upper arm bone.
- Total shoulder replacement is frequently indicated for arthritis with an intact rotator cuff. A reverse shoulder replacement is generally used when arthritis is accompanied by a deficient rotator cuff or for complex fractures.
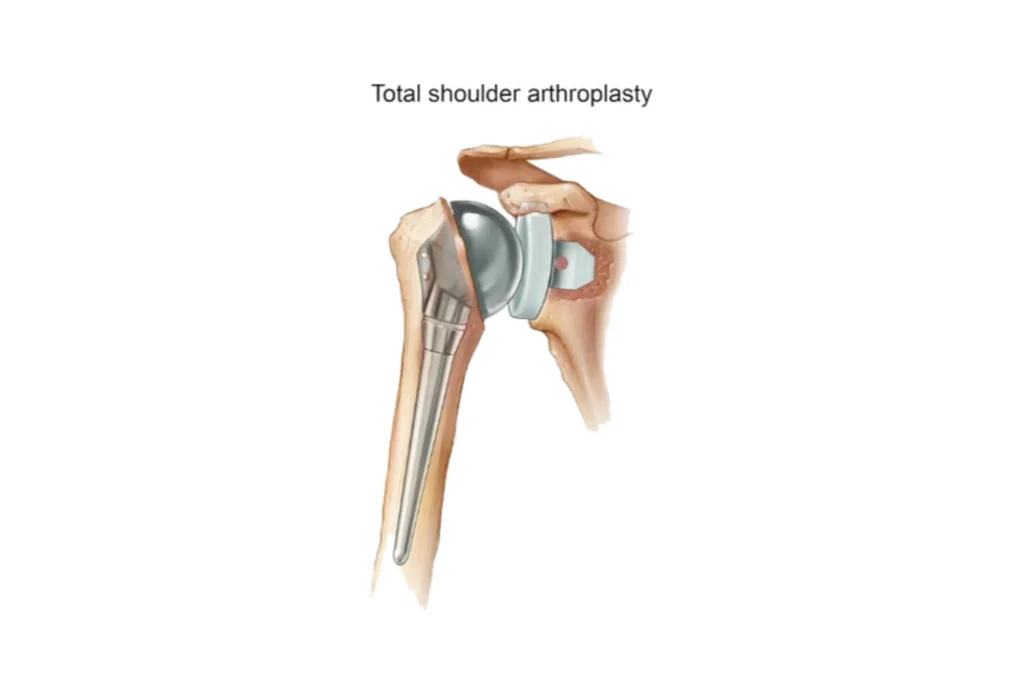
Anatomic Total Shoulder Arthroplasty
Total shoulder replacement, or arthroplasty, is a long-standing treatment option for end-stage glenohumeral arthritis when the rotator cuff is healthy, intact and functional. It has provided significant pain relief and functional improvement to many patients over the years.
The term “anatomic” is key to understanding this procedure. The goal of total shoulder replacement is to replicate the shoulder’s natural anatomy as closely as possible. The shoulder joint is a ball-and-socket joint. The “ball” is the head of the humerus (upper arm bone), and the “socket” is the glenoid, a shallow dish on the shoulder blade.
During a total shoulder replacement, the surgeon removes the damaged surfaces of the joint. They replace the humeral head with a smooth, metal ball component, which is often secured to the humerus with a stem. The glenoid socket is resurfaced with a smooth, durable plastic component.
Indications for Total Shoulder Arthroplasty
The decision to proceed with a total shoulder replacement is generally guided by the underlying pathology and the condition of the surrounding soft tissues. The most common indication is severe, debilitating osteoarthritis of the shoulder. Osteoarthritis is a degenerative joint disease where the cartilage that cushions the ends of the bones wears away.
Other conditions that may lead to a total shoulder replacement include:
- Rheumatoid Arthritis: This is an inflammatory type of arthritis that can destroy both the cartilage and the bone.
- Post-Traumatic Arthritis: Arthritis that develops after a serious shoulder injury, such as a fracture or dislocation.
- Avascular Necrosis (AVN): A condition where the blood supply to the humeral head is disrupted, causing the bone to die and collapse.
Expected Outcomes and Recovery
Many patients who undergo total shoulder replacement experience a reduction in pain. Functional improvement is also often substantial, with many patients regaining range of motion.
The recovery process involves a structured physical therapy program. Many patients may return to light activities within a few weeks and more strenuous activities, such as golf or swimming, after several months, following their surgeon’s guidance. Certain activities may be restricted long-term to protect the new joint.
Reverse Total Shoulder Arthroplasty
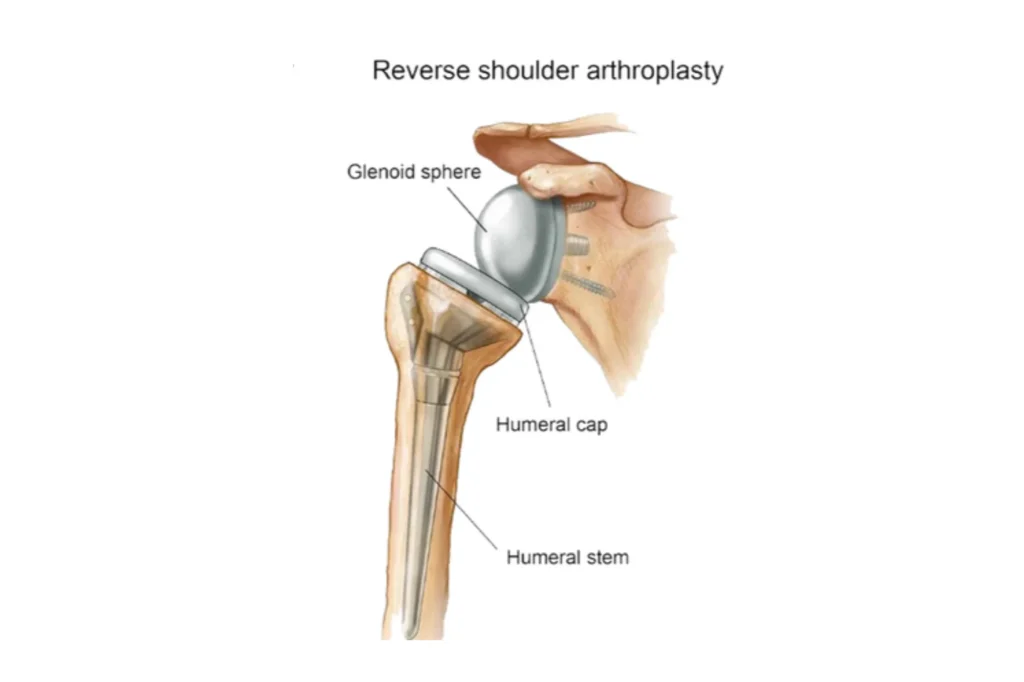
The name “reverse” describes the procedure’s core concept: the natural ball-and-socket anatomy is inverted. Unlike in a traditional total shoulder replacement, the metal ball component is fixed to the glenoid, and the plastic socket component is fixed to the top of the humerus.
By moving the center of rotation of the joint medially (closer to the body) and distally (further down the arm), the reverse design allows the deltoid muscle to compensate for the rotator cuff. In a reverse replacement, the deltoid may function effectively even when the rotator cuff is severely damaged.
Indications for Reverse Total Shoulder Arthroplasty
The primary and most common indication is rotator cuff tear arthropathy (CTA). This is a severe condition where a massive, irreparable tear of the rotator cuff leads to chronic instability, superior migration of the humeral head, and arthritis.
Other potential indicators for reverse shoulder replacement include:
- Massive, Irreparable Rotator Cuff Tears: Patients with a large tear that cannot be surgically repaired and who have functional loss.
- Complex Proximal Humerus Fractures: Especially in older patients with poor bone quality, where traditional fixation methods may not be successful.
- Chronic Shoulder Instability: Certain severe cases of instability that have failed other treatments.
Expected Outcomes and Recovery
The main goal of reverse shoulder replacement is to restore functional arm elevation and provide reliable pain relief. Many patients who could not lift their arm before surgery may regain the ability to raise their arm to shoulder level or higher, allowing them to better perform daily activities like dressing, reaching into a cupboard, and personal hygiene.
The recovery is similar to a total shoulder replacement, frequently requiring a dedicated physical therapy regimen. However, the focus of the early rehabilitation is often different, emphasizing the protection of the subscapularis tendon (if it was repaired) and the careful strengthening of the deltoid muscle.
The Patient Selection Process: When to Choose Which
The decision-making process is a collaborative effort between the patient and an experienced orthopedic surgeon. It generally involves a thorough physical examination, a detailed review of the patient’s medical history, and imaging tests.
The integrity of the rotator cuff is an important factor in determining the appropriate procedure.
- Intact Rotator Cuff: If the rotator cuff is healthy and the primary problem is pain and stiffness from arthritis, a total shoulder replacement may become the procedure of choice.
- Deficient Rotator Cuff: If the patient has a massive, irreparable rotator cuff tear, especially one that has led to arthritis, a reverse shoulder replacement may be the better choice.
Beyond the rotator cuff, several other patient-specific factors influence the final decision, including age, activity level, bone quality, and previous surgical procedures.
Summary
The decision between a reverse total shoulder vs total shoulder replacement is an important decision rooted in a careful assessment of the patient’s unique anatomy and pathology. The total shoulder arthroplasty has been shown to be generally effective in treating severe arthritis when the rotator cuff is functional. The reverse shoulder arthroplasty is an innovative option for the complex problem of arthritis combined with a deficient rotator cuff.
Both procedures represent a potential opportunity to alleviate chronic pain and restore meaningful function. By engaging in an open, detailed discussion with your orthopedic surgeon, you can choose the procedure that is best suited to your specific condition and your personal goals for recovery and activity.
Frequently Asked Questions
Can I still play sports or lift heavy objects after a shoulder replacement?
The ability to return to sports and heavy lifting depends on the type of replacement and the surgeon’s recommendations. Many patients can return to low-impact sports like golf, swimming, and tennis. High-impact activities or those involving repetitive heavy lifting may be discouraged to protect the implant from wear.
How long does the recovery process take before I feel “normal” again?
While the initial recovery is a matter of weeks, the full recovery process is a marathon, not a sprint. Many patients require a structured physical therapy program for at least three to six months to maximize their range of motion and strength. It may take six months to a full year or longer before a patient feels they have reached their maximum potential and can truly feel “normal” again, with the new joint fully integrated into their daily life.
What are the risks or complications of shoulder replacement surgery?
As with any major surgery, risks include infection, nerve injury, stiffness, implant loosening, or dislocation. These complications are relatively uncommon. Following your surgeon’s instructions carefully during pre-operative planning and recovery may help minimize risk.