Shoulder Disorders Detroit, MI
(248) 952-8080
1560 E Maple Rd
Suite 120
Troy, MI 48083
Monday - Friday | 8:00 AM - 5:00 PM
Specialties
Discover Recent Posts
Shoulder pain can limit everyday activities, from reaching overhead to carrying groceries or playing sports. Because the shoulder is one of the most mobile joints in the body, it is also more prone to injury and wear. Dr. Shariff K. Bishai provides advanced care for a wide range of shoulder disorders to help patients in the Detroit area regain strength, motion, and confidence in their shoulder function.
Shoulder Anatomy
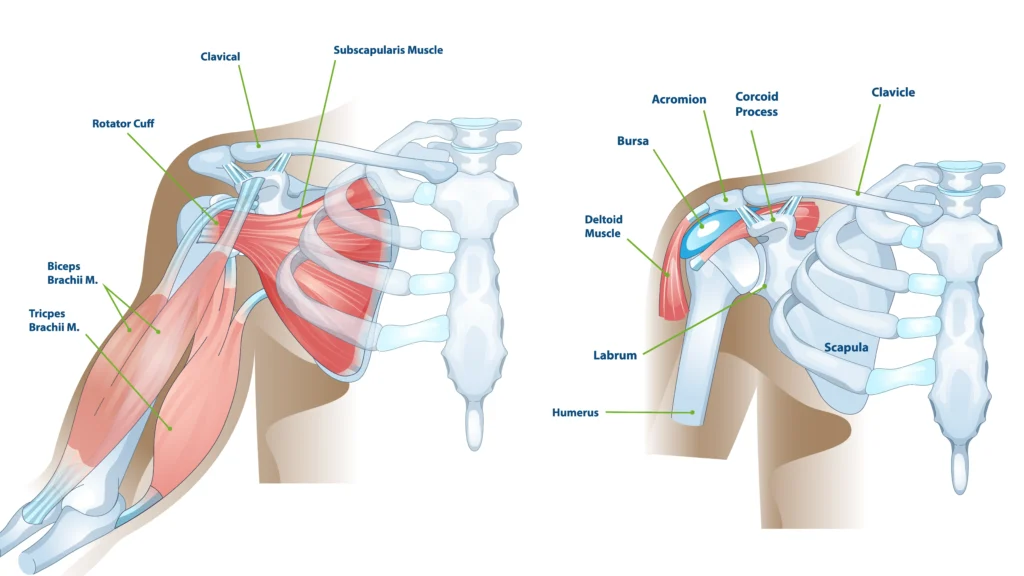
The shoulder is a ball-and-socket joint where the humerus meets the scapula, with the clavicle adding stability at the top of the joint. This arrangement allows the arm to move in nearly every direction. The rotator cuff is a group of muscles and tendons that keep the head of the humerus properly centered as it rotates within the glenoid socket of the scapula. The labrum is a rim of cartilage that deepens the socket and contributes to stability, especially during overhead motion.
Supporting the joint are strong ligaments that connect bone to bone and provide stability, while tendons attach muscle to bone and transmit power for motion. The bursae are fluid-filled sacs that reduce friction between structures during movement. The balance of all these tissues allows for remarkable mobility, but it also leaves the shoulder more prone to injury, instability, and degenerative changes over time.
Common Shoulder Disorders
Rotator Cuff Tears
A rotator cuff tear occurs when one or more of the tendons of the rotator cuff become partially or completely torn. This can develop after a sudden injury, such as a fall, or gradually from repetitive overhead activities and age-related wear. Patients often experience shoulder weakness, night pain, and difficulty lifting or rotating the arm.
Treatment may begin with rest, physical therapy, and anti-inflammatory measures to improve strength and reduce pain. If symptoms persist or the tear is large, arthroscopic or open surgical repair may be recommended. Recovery involves a structured rehabilitation program, and most patients gradually regain motion and strength over several months.
Shoulder Instability and Dislocation
Shoulder instability happens when the head of the humerus does not stay firmly within the glenoid socket. This may be due to ligament stretching, labral tears, or repeated dislocations. Some patients feel the shoulder “slip” or “pop out” during activity, while others experience ongoing discomfort and weakness.
Treatment can include targeted therapy to strengthen the muscles around the joint and improve stability. In cases of recurrent dislocation or significant labral injury, arthroscopic stabilization surgery may be recommended. Recovery usually involves a period of rest followed by progressive therapy to restore both stability and range of motion.
SLAP Tears and Labral Injuries
A SLAP tear involves damage to the upper portion of the labrum, which can occur from repetitive overhead movements or trauma. Patients may notice clicking, catching, or pain with certain motions, especially throwing. Labral injuries often interfere with athletic performance and daily activities requiring shoulder stability.
Non-surgical treatments such as rest, medication, and therapy can improve symptoms in some cases. Arthroscopic repair or debridement may be needed for persistent pain or instability. Rehabilitation focuses on restoring shoulder strength, stability, and gradual return to activity.
Frozen Shoulder (Adhesive Capsulitis)
Frozen shoulder develops when the capsule surrounding the joint thickens and tightens, restricting motion. It often appears gradually, sometimes following an injury, surgery, or in association with medical conditions such as diabetes. Patients experience stiffness, significant loss of range of motion, and pain that can interfere with sleep.
Treatment may involve a combination of physical therapy, stretching exercises, and medications to reduce pain and inflammation. In resistant cases, procedures such as manipulation under anesthesia or arthroscopic release can help restore motion. Recovery may take many months, but most patients see significant improvement with dedicated care.
Shoulder Impingement and Bursitis
Shoulder impingement occurs when the tendons of the rotator cuff become irritated as they pass under the acromion, the top part of the shoulder blade. Bursitis, or inflammation of the bursa, often develops alongside impingement. These conditions cause pain with lifting, reaching, or repetitive overhead movement.
Treatment focuses on reducing inflammation and restoring normal mechanics of the joint. Physical therapy, medications, and activity modification are common first steps. If symptoms do not improve, arthroscopic procedures can smooth bone spurs or relieve pressure on the tendons and bursa. Recovery is usually gradual but often successful in returning patients to normal activities.
Shoulder Arthritis
Arthritis of the shoulder develops when the cartilage covering the joint surfaces wears down. This degeneration leads to pain, stiffness, grinding sensations, and loss of mobility. It can develop from age-related wear, prior injury, or inflammatory conditions.
Initial management often includes medications, therapy, and injections to control pain and improve motion. When arthritis becomes advanced and significantly affects quality of life, surgical options such as shoulder replacement may be considered. Recovery times vary, but many patients achieve meaningful improvement in pain and function.
Biceps Tendonitis
Biceps tendonitis occurs when the tendon that connects the biceps muscle to the shoulder becomes inflamed. This often results from overuse, repetitive lifting, or underlying shoulder problems. Patients typically notice pain in the front of the shoulder that worsens with activity.
Most cases respond well to non-surgical treatment such as rest, anti-inflammatory medications, and physical therapy. In more persistent cases, procedures to clean or reattach the tendon may be recommended. With proper care, most patients experience a steady return to normal function.
Total Shoulder Replacement Surgery
Total shoulder replacement surgery may be performed when arthritis or severe degeneration has worn away the smooth cartilage surfaces of the shoulder joint. In this procedure, the damaged surfaces of the humeral head and glenoid socket are replaced with metal and plastic components that aim to restore smooth movement. This approach is typically best suited for patients with intact rotator cuff tendons who continue to have significant pain and stiffness despite conservative treatments.
Recovery involves a short hospital stay or outpatient procedure depending on the case. Early rehabilitation focuses on gentle motion to protect the new joint, followed by strengthening and functional exercises. With consistent therapy, many patients regain mobility, reduce pain, and return to daily activities, enjoying long-term improvements in comfort and function.
Reverse Shoulder Replacement Surgery
Reverse shoulder replacement is designed for patients whose rotator cuff tendons are severely damaged or irreparable, often in combination with arthritis. In this procedure, the normal ball-and-socket structure of the shoulder is reversed: a ball component is attached to the socket and a cup is placed on the humeral side. This design allows the deltoid muscle, rather than the rotator cuff, to power the arm’s movement.
Recovery is similar to total shoulder replacement but may require closer attention to strengthening the deltoid muscle. Patients often experience reduced pain and improved function, even when other treatments have failed. For those with severe rotator cuff damage or complex arthritis, reverse shoulder replacement can provide meaningful improvements in both mobility and quality of life.
Treatment & Recovery
Treatment for shoulder disorders begins with a careful evaluation to understand the specific cause of pain. Conservative measures such as physical therapy, medications, and activity modification are often effective, especially in early stages of many conditions. Injections may also provide temporary relief and allow patients to participate in rehabilitation.
When non-surgical approaches are not enough, minimally invasive arthroscopic procedures may be used to repair torn tendons or stabilize the joint. For advanced arthritis or complex injuries, total or reverse shoulder replacement may be the most effective solution.
Recovery varies depending on the disorder and the treatment chosen, but a dedicated rehabilitation program is always essential to restore motion, strength, and stability. With appropriate care, many patients return to work, sports, and daily activities with lasting improvement.
Shoulder pain can be one of the most difficult problems to live with, limiting independence, disrupting sleep, and keeping patients from the activities they enjoy most. Choosing an experienced specialist makes a difference in achieving the best outcome.
Dr. Bishai is board certified in orthopedic surgery and sports medicine and has advanced fellowship training in both open and arthroscopic techniques. He is dedicated to providing patient-centered care for shoulder disorders, combining clinical expertise with a focus on helping each patient return to an active, pain-free life.



