A broken shoulder is a common injury that can significantly impact a patient’s quality of life, limiting mobility and causing pain. Patients facing this injury may wonder how to treat a broken shoulder. Given the shoulder’s complex anatomy and its important role in nearly every upper body movement, understanding the nature of the injury and the spectrum of available treatments is the first step toward recovery. In this post, we’ll take a close look at the causes, types, diagnostic process, and modern treatment strategies for a fractured shoulder.
Key Takeaways
- A broken shoulder typically involves one of three bones: the humerus (upper arm bone, most common), the clavicle (collarbone), or the scapula (shoulder blade, least common). The type of fracture guides the treatment approach.
- High-energy trauma (such as car accidents or sports injuries) often causes fractures, while in older adults, low-energy falls, especially those linked to osteoporosis, are a common cause.
- Many shoulder fractures may be successfully treated non-surgically with immobilization, pain management, and early physical therapy. Surgery is typically recommended for significantly displaced, unstable, or open fractures.
Understanding the Anatomy of a Broken Shoulder
The shoulder is one of the most mobile and complex joints in the human body, formed by the humerus, scapula, and clavicle in a ball-and-socket configuration. A fracture can occur in any of these bones.
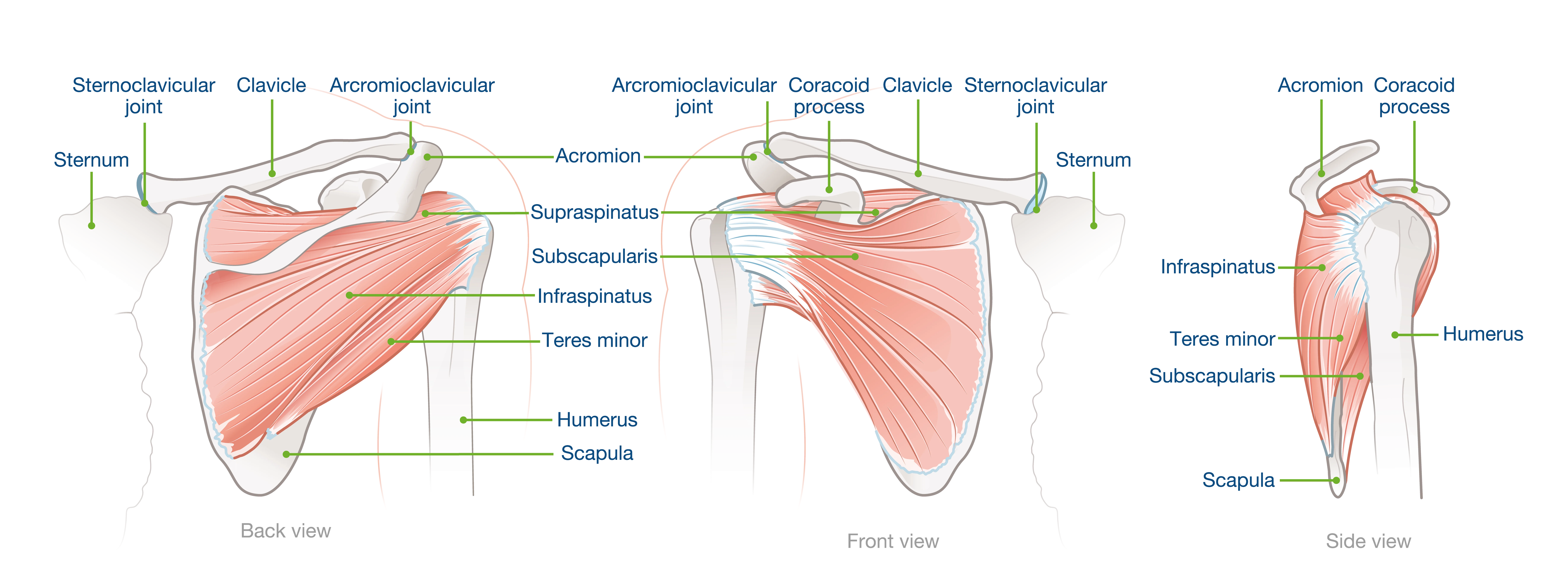
The proximal humerus, or upper arm bone, is the most common site of a shoulder fracture, particularly among older adults with reduced bone density (osteoporosis) who experience a fall onto an outstretched arm. The Neer classification system categorizes fractures in this area by dividing the bone into four parts (the head, greater tuberosity, lesser tuberosity, and shaft) and determining how many of these parts are displaced.
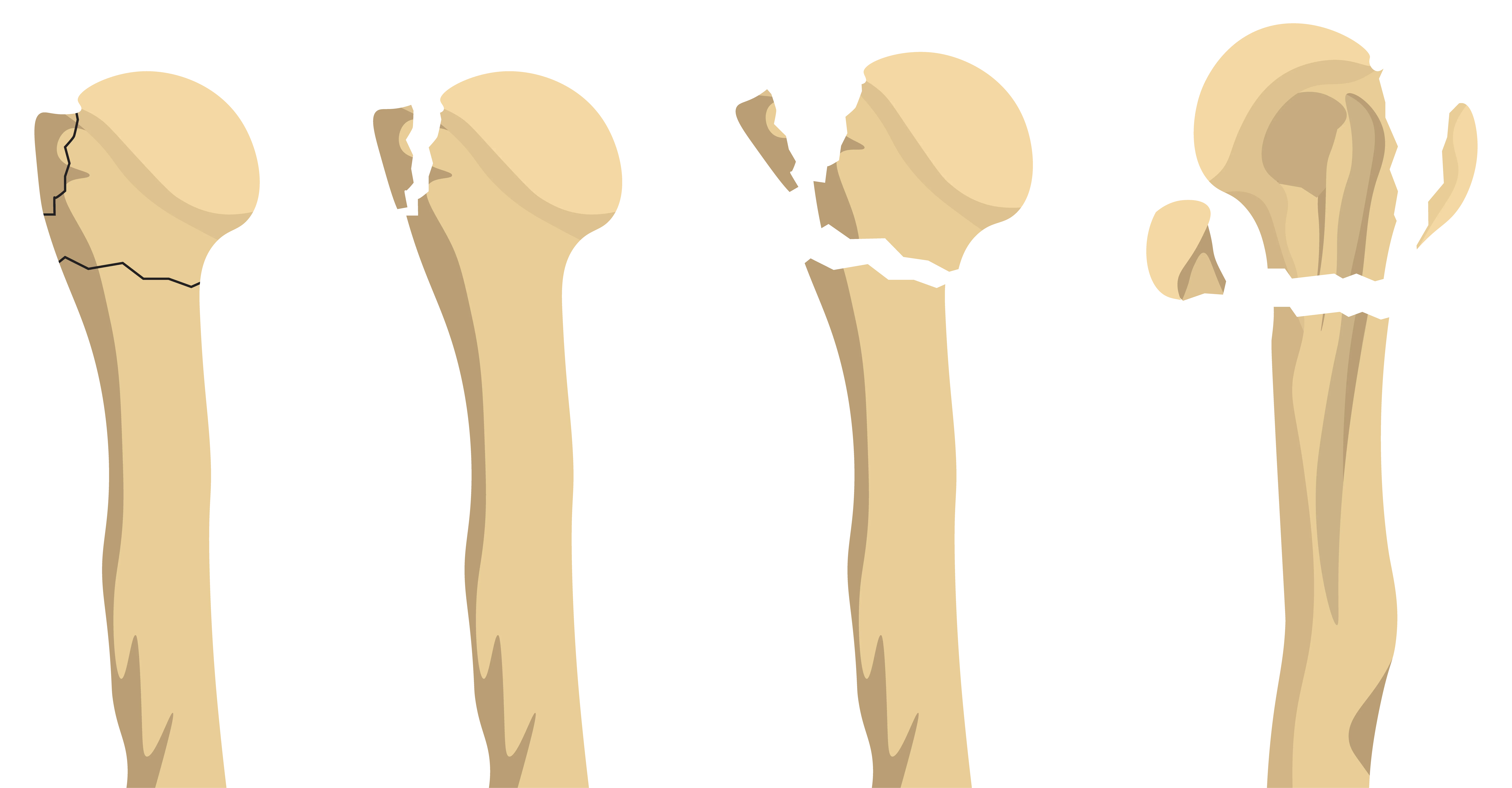
The clavicle, or collarbone, is another frequent site of injury. It is especially vulnerable in contact sports or when someone falls directly onto the shoulder. Most clavicle fractures occur in the middle third of the bone. Fractures of the scapula, or shoulder blade, are rare, representing less than one percent of all fractures. The scapula is well protected by muscles and the ribcage, so breaking it usually requires a high-impact injury or fall.
The Diagnostic Process
An accurate diagnosis is the first step in deciding how to treat a shoulder fracture. An experienced shoulder specialist will typically take a step-by-step approach that includes both a physical examination and imaging tests to fully understand the injury.
During the physical examination, your doctor will look for any obvious signs of injury, such as visible deformity or a “tenting” of the skin, which can occur with certain clavicle fractures. Swelling and bruising are also common and may extend down the arm and chest.
After the examination, the doctor may order imaging tests to confirm the diagnosis and plan treatment. Standard X-rays are the first step, showing bone alignment and any displacement. For more complex injuries, especially those involving the joint surface or shoulder blade, a CT scan can provide a detailed, three-dimensional picture of the fracture, helping the surgeon plan any necessary procedure. An MRI can detect soft tissue injuries like rotator cuff or labral tears that may affect treatment.
Treatment Strategies: Non-Surgical vs. Surgical
The choice between non-surgical (conservative) and surgical treatment depends on several factors, including the fracture type, degree of displacement and stability, and the patient’s age, overall health, and functional demands.
Non-Surgical Treatment (Conservative Management)
Many shoulder fractures, especially non-displaced or minimally displaced proximal humerus fractures and most mid-shaft clavicle fractures, can often heal successfully without surgery. Conservative management focuses on protecting the shoulder while allowing natural healing to occur, followed by a gradual return to motion and strength.
Immobilization involves keeping the arm still in a sling, shoulder immobilizer, or specialized brace. This limits movement so the bone can begin to heal. The immobilization timeline may depend on how stable the fracture is. Pain management is also an important part of early recovery. Non-steroidal anti-inflammatory drugs (NSAIDs) may be used to control discomfort. Ice application helps reduce pain and swelling.
Once the initial healing phase begins, early motion often becomes important to prevent stiffness. A physical therapist may introduce gentle exercises, such as passive range-of-motion and pendulum movements.
Surgical Treatment (Operative Management)
Surgeons may recommend surgery when the shoulder fracture is unstable, the bones shift out of place, the joint surface is involved, or non-surgical treatment is unlikely to restore normal movement. The goal of surgery is to realign and stabilize the bones so they can heal properly.
One common procedure is called open reduction and internal fixation (ORIF). In this surgery, the surgeon makes an incision to move the broken pieces of bone back into their correct position, then uses metal plates and screws to hold them together while they heal. This approach is often used for displaced fractures of the upper arm bone (proximal humerus), collarbone (clavicle), or shoulder blade (scapula).
In more severe cases, when the bone shatters or the blood supply to the ball of the shoulder (humeral head) becomes compromised, surgeons may consider a shoulder replacement. A common procedure type for complex fractures is a reverse total shoulder replacement. In this procedure, the surgeon reverses the normal positions of the ball and socket, placing the ball on the shoulder blade and the socket on the upper arm bone. This design allows the deltoid muscle to lift the arm even if the rotator cuff is weak or torn.
No matter which treatment is used, rehabilitation typically plays a key role in recovery. Physical therapy helps restore flexibility, strength, and coordination once the bone begins to heal.
Phases of Rehabilitation
While timelines and steps may vary, a typical rehabilitation protocol can be divided into phases, guided by the surgeon and physical therapist:
First Phase: Passive Range of Motion
- Goal: Protect the healing fracture and prevent stiffness.
- Activities: The therapist moves the patient’s arm without the patient using their own muscles (passive motion). Pendulum exercises are often started early. No lifting or active use of the arm is permitted.
Second Phase: Active Range of Motion
- Goal: Regain active control of the arm and increase mobility.
- Activities: The patient may begin to move their arm on their own, without assistance. Gentle strengthening exercises for the rotator cuff and scapular stabilizers often begin with light resistance bands or very light weights.
Third Phase: Strengthening and Return to Activity
- Goal: Restore strength, endurance, and return to sports or heavy labor.
- Activities: Progressive resistance training may be intensified. Functional exercises that mimic work or sport-specific movements are incorporated. Full recovery, especially for high-demand activities, can take 6 to 12 months or longer.
Summary
Treating a broken shoulder is a journey that requires a partnership between the patient and a specialized orthopedic team. While the injury can be daunting, the good news is that modern orthopedic care offers many evidence-based treatment pathways. Whether your path involves non-surgical management with a focus on early, controlled motion or a complex surgical reconstruction like a reverse total shoulder arthroplasty, the ultimate goal remains the same: to alleviate pain, restore the intricate mechanics of the shoulder joint, and return you to the activities you enjoy.
Frequently Asked Questions (FAQs)
How long will I have to wear a sling for a broken shoulder?
The duration of sling use is highly dependent on the type and stability of the fracture. For some non-displaced proximal humerus and clavicle fractures, the sling may be worn for around 4 weeks to allow the initial healing to begin. Your doctor will provide a precise timeline based on your specific injury and healing progress.
Will I need surgery for my broken shoulder?
Many broken shoulders do not require surgery. Surgeons reserve surgery for fractures that displace significantly, remain unstable, involve the joint surface, or occur in younger, highly active patients who need precise anatomical alignment to return to demanding activities. A shoulder specialist can evaluate your injury and recommend if surgery may be an appropriate treatment option for you.
When can I start physical therapy, and how long will it take?
Gentle, passive motion exercises often begin within 2 to 4 weeks after the injury, even while the fracture is still healing, to prevent the shoulder from freezing up. The entire rehabilitation process, from injury to maximum functional recovery, can take 6 to 12 months, depending on the severity of the fracture. Unfortunately with some fractures there is a loss of range of motion.




