For many patients, shoulder replacement surgery may help reduce pain and improve shoulder function in people with conditions such as severe shoulder arthritis, rotator cuff damage, or complex fractures. Most patients head into surgery focused squarely on shoulder pain as the primary concern, and understandably so. However, some patients are surprised to experience bicep pain after shoulder replacement surgery.
The reassuring news is that some degree of bicep discomfort following shoulder arthroplasty can occur during recovery and often improves with time and appropriate rehabilitation. That said, understanding what’s typical versus what may require follow-up care is important.
Key Takeaways
- Bicep pain after shoulder replacement surgery is relatively common and often resolves with time and proper rehab.
- The biceps tendon runs through or near the shoulder joint, making it vulnerable to irritation during and after surgery.
- Not all bicep pain is equal, and persistent or worsening pain should be evaluated by your surgeon.
- Physical therapy and activity modification may play a key role in managing post-operative bicep discomfort.
Why Does the Biceps Tendon Get Involved?
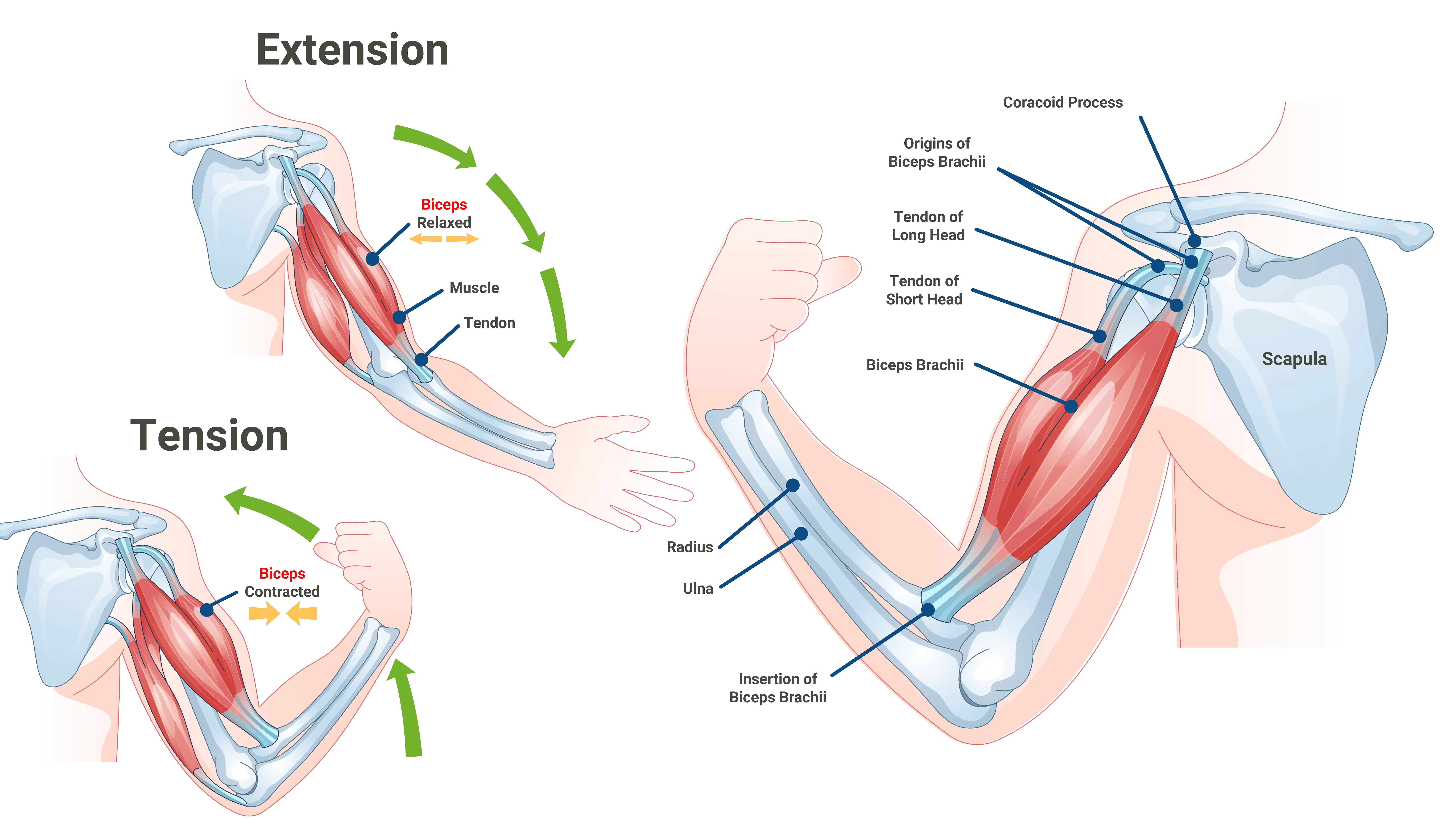
To understand why bicep pain shows up after shoulder surgery, it helps to know a little about shoulder anatomy. The shoulder is a complex ball-and-socket joint made up of three bones: the humerus (upper arm bone), the scapula (shoulder blade), and the clavicle (collarbone). The rotator cuff tendons, the joint capsule, and the biceps tendon all work together to stabilize and move the shoulder.
Specifically, the long head of the biceps tendon (LHBT) originates at the top of the shoulder joint, attaching to the superior glenoid labrum and the supraglenoid tubercle of the scapula. From there, it travels out of the joint and through a groove in the upper humerus called the bicipital groove. Because this tendon runs directly through the shoulder joint and close to the operative field during shoulder replacement surgery, it can experience irritation, inflammation, or structural changes as a result of the procedure.
Surgeons frequently decide how to manage the long head of the biceps tendon as part of the procedure. Options may include leaving the tendon in place, performing a biceps tenotomy (releasing the tendon from its attachment), or performing a biceps tenodesis (reattaching the tendon in a new location).
What Causes Bicep Pain After Shoulder Replacement Surgery?
Bicep pain after shoulder replacement surgery can stem from several different sources. Understanding the potential causes may help you have a more productive conversation with your surgical team.
- Biceps tendon irritation: Even without a specific surgical decision about the tendon, manipulation of the shoulder during surgery can irritate the long head of the biceps. This tends to produce a dull, aching discomfort along the front of the upper arm in early recovery.
- Biceps tenotomy: When the surgeon releases the biceps tendon, patients may notice a change in upper arm contour (sometimes called a “Popeye” deformity), along with temporary aching or cramping in the upper arm. This generally improves over the weeks following surgery.
- Biceps tenodesis: If the tendon was reattached during the procedure, the tenodesis site can be a source of pain while it heals. This pain may feel sharp with certain movements and tends to present along the upper arm or near the shoulder.
- Scar tissue formation: As the body heals, scar tissue may develop around the bicipital groove or in the area of the surgery, potentially creating a pulling or aching sensation in the bicep region.
- Referred pain: Pain originating in the shoulder joint, the rotator cuff, or surrounding soft tissue can sometimes be felt in the bicep area, even when the bicep itself is not the primary source of the problem.
- Nerve irritation: Surgical manipulation may occasionally cause temporary irritation of nerves that supply sensation to the bicep region, leading to aching, burning, or numbness in the upper arm.
Total Shoulder vs. Reverse Shoulder Replacement: Does the Type Matter?
Both total (anatomic) shoulder replacement and reverse shoulder replacement can be associated with bicep pain during recovery, though the mechanisms can differ depending on the procedure.
In a total shoulder replacement, also called anatomic shoulder arthroplasty, the goal is to restore the natural anatomy of the shoulder joint. Both the humeral head (the ball) and the glenoid (the socket) are replaced with implants designed to replicate the shoulder’s normal shape. Because the rotator cuff is still functional in patients who undergo this procedure, the biceps tendon generally remains in a more anatomically familiar environment post-surgery, though it can still be a source of discomfort.
Reverse shoulder replacement is typically recommended for patients with large rotator cuff tears, cuff tear arthropathy, or in certain patients with complex shoulder fractures. In this procedure, the ball-and-socket configuration is intentionally reversed. The ball is placed on the glenoid side and the socket on the humeral side. This shift in mechanics changes the way surrounding soft tissues are tensioned and loaded during shoulder movement. Some reverse shoulder replacement patients report bicep cramping or aching during recovery, which may be related to changes in shoulder mechanics following the procedure.
Regardless of the procedure type, bicep-related discomfort can occur during recovery for some patients. An experienced shoulder surgeon can offer guidance on what to expect based on your specific anatomy and the type of replacement performed.
The Role of Implant Design in Recovery
The design of the shoulder implant itself may influence how surrounding tissues, including the biceps, respond to surgery. I use the InSet® Shoulder System by Shoulder Innovations, a titanium alloy implant system available in both total and reverse configurations.
For total shoulder patients, the InSet® system works to replicate natural shoulder anatomy and restore rotator cuff balance. For reverse shoulder patients, the system’s extensive implant options allow me to tailor the component configuration to each patient’s unique anatomy. This level of customization allows surgeons to adjust implant configuration based on a patient’s anatomy.
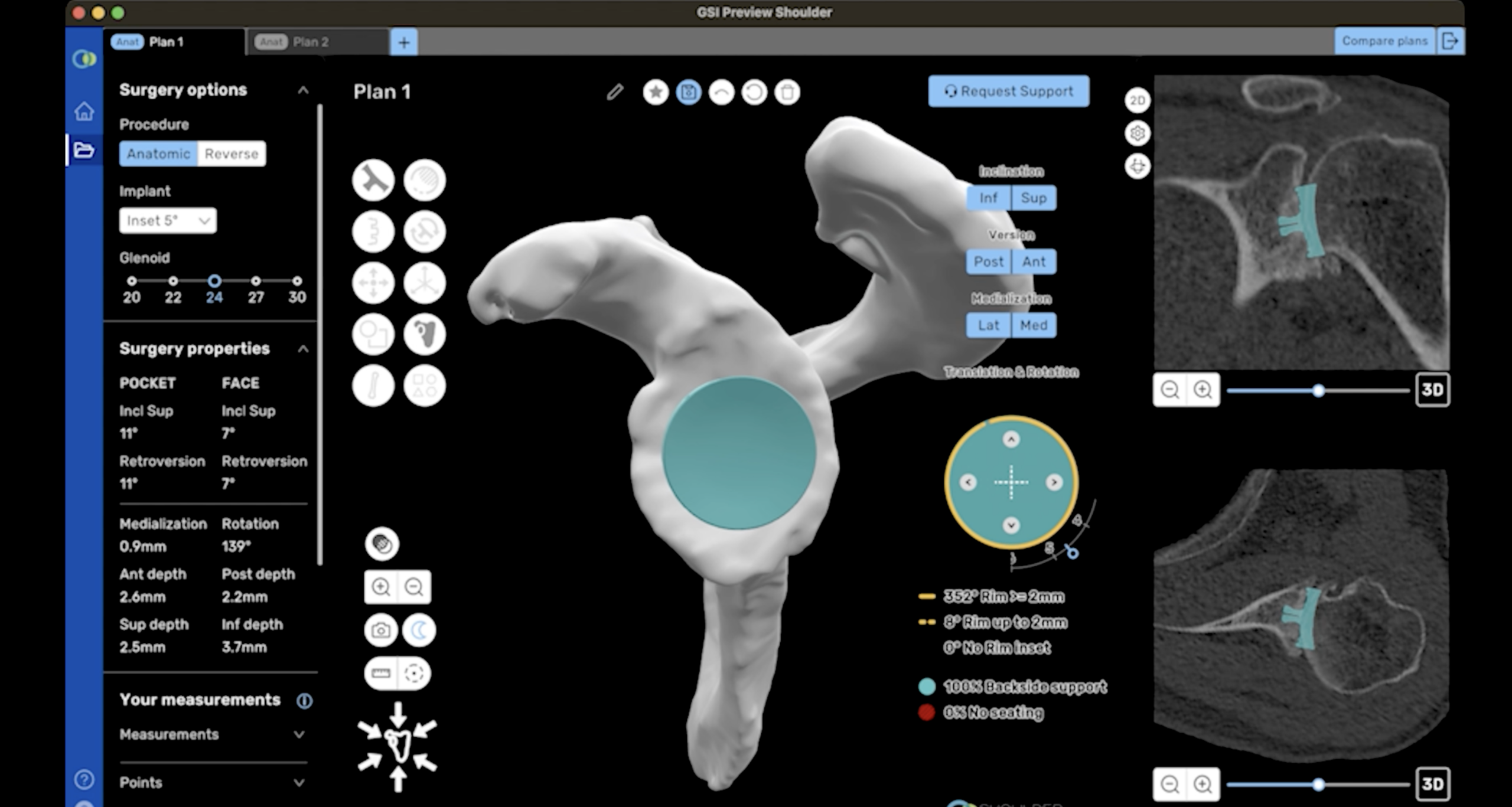
I also use ProVoyance®, a 3D computerized planning software. It converts a CT scan into a virtual 3D model of the patient’s shoulder, allowing me to plan implant sizing and positioning before stepping into the operating room. Thoughtful pre-surgical planning like this may contribute to more predictable outcomes and a more comfortable recovery overall.
Normal Recovery vs. When to Be Concerned
Mild to moderate bicep discomfort in the weeks following shoulder replacement surgery tends to be a normal part of the healing process. The shoulder contains a significant amount of soft tissue, and it needs time to adapt to its new anatomy. Many patients notice gradual improvement in bicep discomfort during the first several weeks to months of recovery. That said, certain signs may suggest you should contact your surgeon’s office rather than wait things out. Consider reaching out if you notice any of the following:
- Bicep pain that worsens significantly after initially improving, rather than following a steady path toward resolution.
- A sudden, sharp pain in the upper arm associated with a specific movement or incident.
- A noticeable popping sensation followed by increased pain and a visible change in upper arm shape.
- Swelling, warmth, or redness around the surgical site paired with increasing bicep discomfort.
- New or worsening numbness, tingling, or weakness developing in the arm or hand over time.
These symptoms don’t automatically point to a serious problem, but they do suggest your surgeon should take a closer look. Early evaluation can rule out issues like biceps tendon rupture, infection, or nerve involvement, and it gives your care team the opportunity to adjust your plan if needed.
Managing Bicep Pain During Recovery
There are several approaches that may help reduce bicep pain after shoulder replacement surgery and support a smoother recovery overall.
Completing your physical therapy program is one of the most impactful steps you can take. The goal of PT is to help restore strength, range of motion, and coordination in the shoulder and surrounding musculature, including the biceps. Following the recommended rehabilitation program helps support recovery and may reduce ongoing discomfort.
Activity modification also tends to matter quite a bit. In the early weeks, avoiding activities that place excessive load on the biceps can help reduce irritation at the surgical site. Your surgeon or physical therapist can guide you on which activities are appropriate at each stage of recovery.
Ice application to the upper arm and shoulder region may help manage swelling and reduce pain, particularly in the early post-operative period. Nonsteroidal anti-inflammatory medications (NSAIDs) or other prescribed pain management options may be recommended by your surgeon when appropriate. Above all, allowing adequate time for healing and resisting the urge to rush back to full activity helps support the best long-term outcomes.
Summary
Experiencing bicep pain after shoulder replacement surgery is more common than many patients anticipate, and it can arise from a variety of sources. Both total shoulder and reverse shoulder replacement patients may notice this type of discomfort, and for most people, it gradually improves with time, structured physical therapy, and appropriate activity management. If you’re experiencing bicep pain following shoulder surgery, whether it feels routine or something seems off, the most important step is to stay in communication with your surgical team.
Frequently Asked Questions
Is it normal to have bicep pain after shoulder replacement surgery?
Yes, some degree of bicep discomfort is relatively common following shoulder arthroplasty. The biceps tendon runs through the shoulder region and can be affected by surgical manipulation, tissue inflammation, or changes in shoulder mechanics after surgery. For most patients, this pain gradually improves over the course of recovery, particularly with consistent physical therapy and appropriate activity modifications.
How long does bicep pain typically last after shoulder replacement?
The timeline tends to vary from patient to patient. Many people notice meaningful improvement in bicep discomfort within the first 6 to 12 weeks following surgery. Others may experience some lingering discomfort for several months, particularly if the biceps tendon was directly addressed during the procedure through a tenotomy or tenodesis, as the healing process at that site may take longer.
What is a biceps tenodesis, and why might my surgeon perform it during shoulder replacement?
A biceps tenodesis is a procedure in which the long head of the biceps tendon is released from its original attachment point inside the shoulder joint and reattached in a new location, typically lower on the humerus. Surgeons may perform this procedure during shoulder replacement when the biceps tendon is already irritated or damaged, or when addressing the tendon may reduce the likelihood of persistent anterior shoulder pain after surgery.




